Osteoporosis Treatments You Need To Know About

3 Natural Osteoporosis Treatments
“Adequate calcium & vitamin D throughout life, as part of a well-balanced diet, may reduce the risk of osteoporosis.”
Get These 3 Things To Increase Your Bone Density
The best way to protect yourself against osteoporosis is by taking preventative steps. According to the FDA, getting enough calcium and vitamin D as part of a balanced diet throughout your life can help lower the risk of developing osteoporosis.
But what if you’ve already developed osteoporosis? Does that mean it’s too late to increase your bone density? Clinical studies say, “no!” The fact is that a few small changes in your lifestyle can stop bone loss and actually increase your bone density.

What is Osteoporosis?
Osteoporosis, “porous bones“, is a disease that causes bones to become brittle and very susceptible to fractures.1 These fractures typically occur in the hip, spine, and wrist. A fracture or broken bone can have a huge effect on your life, causing disability, pain, or loss of independence. Fractures can make it very difficult to do daily activities without help. And unfortunately, the International Osteoporosis Foundation currently estimates that 1 in 3 women and 1 in 5 men over age 50 will suffer an osteoporotic fracture.2
Osteoporosis Causes and Risk Factors
From age 40 and on we lose about 1% of our bone density each year!³ With that said, you should be aware of the litany of causes and risk factors that can increase your chances of osteoporosis.
The Top Causes of Osteoporosis
Be on the lookout for the following osteoporosis triggers. Some will come as no surprise. But others just might. Here are some predictable causes:
However, there are others. Here’s a handy visual guide to some of the top osteoporosis triggers.
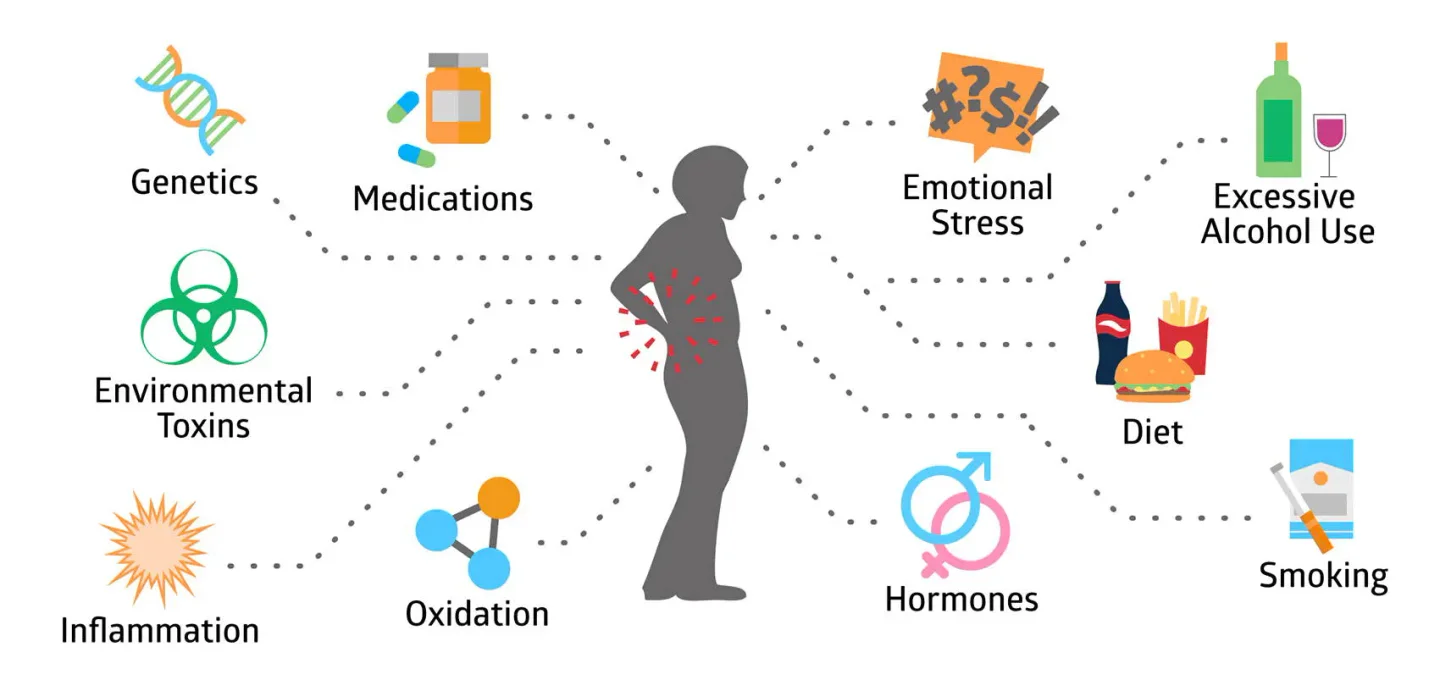
Natural Ways To Increase Bone Density
#1 - Get Plenty Sleep
Studies have shown that a lack of sleep can affect your bone health by impacting how bones repair themselves.[1] Your bones, like most other parts of your body, have a built-in way of healing themselves. Most of this work is done by cells called Osteoclasts (these are the cells that remove old and damaged bone) and Osteoblasts (these are the cells that build healthy new bone). Studies show that sleep deprivation interferes with the activity of these essential cells. So do your bones a favor, and get plenty of good quality sleep.
#2 - Get Plenty Exercise
If you want to protect your bones from age-related weakening, here’s welcome news. Studies show that specific physical exercises help prevent bone loss. In fact, they can even stimulate your bones to become stronger. Scientists call this ‘Wolf’s Law.’ And it explains why having frail bones doesn’t have to be an inevitable part of aging. Because your bones are living tissues, they’ll become stronger the more you use them. That’s why studies show that regular weight-bearing exercise is a great way to protect your bone health. [2]
#3 - Get Plenty Nutrients
Exercise is great for bone health, but your bones need nutrients too. A study - published in The International Journal of Medical Science[3] - found that 16 bone-building nutrients can stop bone loss from happening. In fact, researchers discovered that by adding these nutrients to your diet, your bones will actually get stronger. Imagine that! Enjoying your life without worrying about fracturing a bone. Want to know more about these essential nutrients?
Click on any of the 16 nutrients below to see how it can help to increase your bone density.
Calcium
Magnesium
Potassium
Boron
Copper
Manganese
Silicon
Strontium
Nickel
Phosphorus
Selenium
Vanadium
Zinc
Vitamin D3
Vitamin K2-7
Vitamin C
Build New Bone Today
Loading...
You Need All These Nutrients. Some Isn’t Enough!
Your bones need all 16 of these bone-supporting nutrients. In fact, lacking a single one of these minerals or vitamins can lower your bone mineral density leaving you vulnerable to fractures. But there’s a problem…
It’s almost impossible to get all 16 of these essential nutrients from your diet alone.
That's why AlgaeCal is so important.
AlgaeCal - a plant calcium - naturally bridges the gap between your diet and the essential nutrients your bones need. And remember, you don’t need some of these nutrients - you need all of them.
That’s why AlgaeCal is the only calcium supplement clinically supported to increase bone density. That’s right. AlgaeCal doesn’t just stop bone loss – it actually increases bone density.
So if you want to increase your bone density, click on one of the links below to get started.
AlgaeCal is Clinically Supported to Increase Bone Density
AlgaeCal Plus is clinically supported to increase your bone density. In one study published in the International Journal of Medical Sciences, 414 postmenopausal women each took different formulations of AlgaeCal Plus for 12 months. The result? The lowest average increase in bone density was 1.3%.12
In another study published in the same journal, 216 men and women took AlgaeCal Plus with our Strontium Boost supplement. In just 6 months, they saw an average increase of over 2% in bone density.13 Don’t forget, we lose bone density every year after age 40. And other calcium supplements at best only slow down the bone loss. But AlgaeCal Plus shows outright bone density increases!
Here’s the most amazing part: in AlgaeCal’s most recent clinical study, 172 women in their mid-60s increased bone density 7 consecutive years with the AlgaeCal Plus and Strontium Boost combo!14 On average they gained 1% a year, every year. Until now, this sort of result was unheard of. But it’s not only possible with our Bone Builder Packs, it’s guaranteed. No one should suffer from bone loss when we now have the means to naturally reclaim low bone density. It’s preventable when you know how to protect yourself every day.
Their bones got stronger with AlgaeCal. Yours can too.
YES! I want to build brand-new youthful bone now!
Special Introductory Offer Today + Free US Shipping
Loading...
What is AlgaeCal Plus?
What is Strontium Boost?
Do I have to take both AlgaeCal Plus and Strontium Boost?
What if I have trouble swallowing the capsules?
Does AlgaeCal Plus cause side effects such as deposits in kidneys or arteries?
Can I take AlgaeCal Plus if I am on bone medications?
Does my doctor know about AlgaeCal?
What is the Stronger Bones for Life Guarantee?
Sources
1.Everson CA, Folley AE, Toth JM. Chronically inadequate sleep results in abnormal bone formation and abnormal bone marrow in rats. Experimental biology and medicine. 2012;237:1101-9. doi:10.1258/ebm.2012.012043
2.https://www.osteoporosis.foundation/health-professionals/fragility-fractures/epidemiology
3.https://www.medsci.org/v08p0180.htm
4.70 Year of Soil Depletion. Thomas, D.E. (2003) a study of mineral depletion of foods available to us as a nation over the period 1940 -1991. Nutrition and Health 17: 85-115.
5.Average Mineral Content in Selected Vegetables, 1914 - 1997. Lindlahr, 1994; Hamaker, 1982; US Department of Agriculture, 1963 & 1997
6.Bone and soft tissue proportions change as we age. http://Rodeoderm.com
7.https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7287917/#:~:text=Zinc%20is%20an%20essential%20mineral,and%20regeneration%20are%20poorly%20understood
8.https://www.mayoclinic.org/healthy-lifestyle/nutrition-and-healthy-eating/in-depth/calcium-supplements/art-20047097
9.https://pubmed.ncbi.nlm.nih.gov/28093633/#:~:text=Dietary%20potassium%20may%20neutralize%20acid,older%20men%20and%20postmenopausal%20women
10.https://ods.od.nih.gov/factsheets/VitaminD-Consumer/
11.https://www.mayoclinic.org/drugs-supplements-vitamin-c/art-20363932
12.http://www.ncbi.nlm.nih.gov/pubmed/?term=21448303
13.http://www.ncbi.nlm.nih.gov/pubmed/21492428
14.https://www.ncbi.nlm.nih.gov/pubmed/26885697























