Living with Spinal Osteoporosis
Osteoporosis and Spine Fractures | Causes and Symptoms of Osteoporosis in the Spine | Osteoporosis Spine Exercises | FAQs
If you – or someone you know and love – suffer from the pain and torment of spinal osteoporosis, know these facts:
You are not alone.
There are measures you can take to alleviate your pain.
There are measures you can take to regain bone density, even in your spine.
Today, we will discuss some of the risk factors involved with spinal osteoporosis, the terminology used by the medical community (and what they mean in plain English), measures you can take after diagnosis and even vertebral fracture, plus one thing you can do to help reduce your risk of losing vital vertebral bone density.
Osteoporosis and Spine Fractures
Simply put, the numbers are frightening.
- A 50 year old white woman has a 16% lifetime risk of experiencing a vertebral fracture whereas a 50 year old white man’s lifetime risk is 5%.(1)
- A woman 65 years of age with one vertebral fracture has a one in four chance of another fracture over 5 years, which can be reduced to one in eight by treatment.(2)
- Vertebral fractures can lead to back pain, loss of height, deformity, immobility, increased number of bed days, and even reduced pulmonary function.(3)(4)(5) Their impact on quality of life can be profound as a result of loss of self-esteem, distorted body image and depression.(6)(7)(8)(9) Vertebral fractures also significantly impact on activities of daily living.(10)(11)
- After hospitalization for a vertebral fracture, there is a greatly increased risk of requiring hospitalization for a further fracture in the years following initial hospitalization.(12)
- Women who develop a vertebral fracture are at substantial risk for additional fracture within the next 1-2 years.(13)(14)
- It is estimated that only one-third of vertebral fractures come to clinical attention(15) and under-diagnosis of vertebral fracture is a worldwide problem. The proportion of vertebral fractures that go unrecognized is as high as 46% in Latin America, 45% in North America, and 29% in Europe/South Africa/Australia.(16)
Women, especially those older than 50, are at greatest risk for spine fractures. By age 80, about 40% of women have had a spinal fracture. Estimates put the number of vertebral fractures that occur each year in the United States at about 700,000.
Men can also have a spinal fracture, and women and men who have osteoporosis have an even greater risk of spine fractures.
Age obviously plays a major role in spine fractures. As you age, your bones may become increasingly thinner and weaker. This is what leads to osteoporosis – and when it is focused on the bones in your vertebra, it’s called spinal osteoporosis.
Believe it or not, simply the effort required to just hold your body erect can be enough to cause a spinal fracture when someone has spinal osteoporosis.
Causes and Symptoms of Osteoporosis In The Spine
The pain caused by spinal osteoporosis can affect many areas of your daily life. The pain can range from a sudden, sharp and severe pain from walking or simply standing, to pain and difficulty and pain when you twist, turn or bend.
But when osteoporosis becomes severe, it can lead to fractures and a condition called kyphosis. Kyphosis is a deformity resulting from spinal compression fractures, sometimes described as the “dowager’s hump.” Both fractures and kyphosis can be very painful.
 Most people describe having pain in their bones and muscles, particularly in their back but also hips, arms, ribs and knees.
Most people describe having pain in their bones and muscles, particularly in their back but also hips, arms, ribs and knees.
The level of pain differed and while many people deal with some level of pain on a regular basis it was particularly challenging for those who suffered severe pain due to collapsed vertebrae.
Also it may take longer for people to recover from the emotional effect of pain and normalize their everyday activities again. (Many adults compare themselves with others in their peer group and because they could no longer be as active, their self-esteem was affected.)
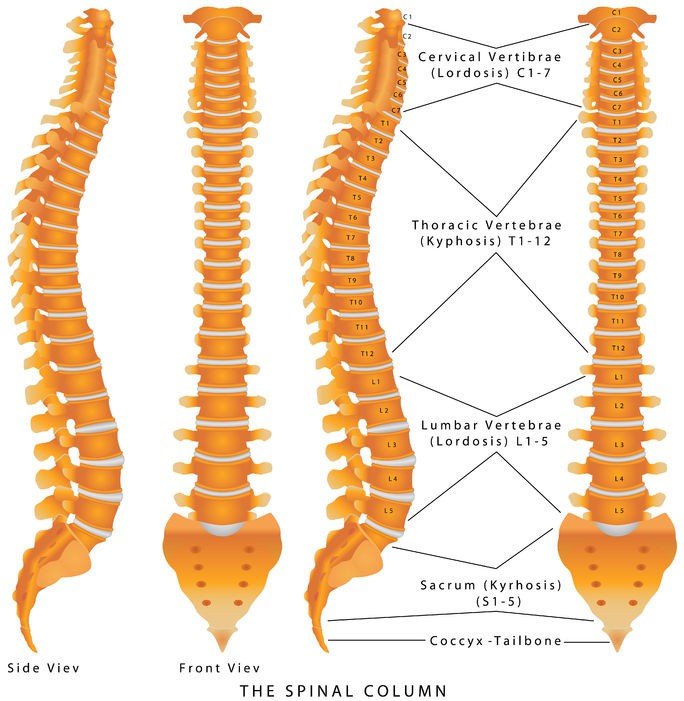
Let’s take a look at a few more terms(17) relevant to your spine.
Centrum – The body of a vertebra.
Cervical – The neck region of the spine containing the first seven vertebrae.
Fatigue Fracture – A fracture that occurs in bone as a result of repeated stress as opposed to a single injury.
Internal Fixation – The immobilization of bone fragments or joints with implants in order to promote healing or fusion.
Lumbar – The lower part of the spine between the thoracic region and the sacrum. The lumbar spine consists of five vertebrae
Minimally Invasive Surgery – Surgery requiring small incision(s), usually performed with tiny cameras.
Spine – The flexible bone column extending from the base of the skull to the tailbone. It is made up of 33 bones, known as vertebrae. The first 24 vertebrae are separated by discs known as intervertebral discs, and bound together by ligaments and muscles. Five vertebrae are fused together to form the sacrum and 4 vertebrae are fused together to form the coccyx. The spine is also referred to as the vertebral column, spinal column, or backbone.
Vertebra – One of the 33 bones of the spinal column. A cervical, thoracic, or lumbar vertebra has a cylindrical shape on one side and an arch on the other. The plural of vertebra is vertebrae.
Osteoporosis Spine Exercises
Can You Ease your Back Pain with Exercise?
A typical response to experiencing back pain is to take it easy – either stay in bed or at least stop any activity that is at all strenuous. While this idea is understandable and may even be recommended in the short term, when done for more than a day or two it can actually undermine healing. Instead, active forms of back exercises are almost always necessary to rehabilitate the spine and help alleviate back pain.
A regular routine of lower back exercises helps you avoid stiffness and weakness, minimize recurrences of lower back pain, and reduce the severity and duration of possible future episodes.
A balanced workout of back exercises should include a combination of stretching, strengthening, and low-impact aerobic conditioning.
Stretching
Keep the following in mind when starting a stretching routine as part of a program of back exercises:
- Wear comfortable clothes that won’t bind
- Stretching should be pain-free; do not force the body into difficult positions
- Move into the stretch slowly and avoid bouncing, which may actually tear muscles
- Stretch on a clean, flat surface that is large enough to move freely
- Hold stretches long enough (20-30 seconds) to allow muscles or joints to become loose
- Repeat the stretch, generally 5-10 times
(If you already have low back pain or neck pain, and before starting any new physical activity, it is best to check with a physician or physical therapist.)
Back Exercise Stretches
Many back pain patients know the feeling of tension in the back, especially first thing in the morning. These stretching back exercises can help bring back some suppleness and increase mobility, decreasing back pain and discomfort.
For a list of simple, safe exercises for osteoporosis of the spine, check out our “Exercises for Osteoporosis of the Spine” post. We provide videos and step-by-step instructions for each exercise!
Osteoporosis Spine FAQ’s
How can spinal osteoporosis be treated?
There are several treatment options:
- Prescription Medications: Doctors may prescribe medication to relieve pain. There is a long list of potential drugs, and most have both benefits and negative side-effects.
- Exercise: Several exercise options appear above. Check with your doctor before starting a new fitness program.
- Strontium Treatment for Osteoporosis: If you are concerned about the bone-thinning disease osteoporosis, one treatment you may have heard of and considered is strontium. It has an excellent history of building bone density.
Osteoporosis Myth: Once You Get Osteoporosis, No Treatment Helps
If diagnosed, osteoporosis can be treated with a variety of new osteoporosis medications and supplements that help to prevent bone loss and rebuild bone. These osteoporosis treatments (such as AlgaeCal Plus and Strontium Boost) can substantially reduce your risk of developing dangerous and potentially deadly bone fractures.
What does a fractured vertebrae look like?
When more pressure is put on a bone than it can stand, it will break. The most common type of spine fracture is a vertebral body compression fracture (below.) Sudden downward force shatters and collapses the body of the vertebrae. If the force is great enough, it may send bone fragments into the spinal canal, called a burst fracture.
What is a vertebral fracture?
A vertebral compression fracture occurs when the block-like part of an individual bone of the spine (vertebra) becomes compressed due to trauma. Usually the trauma necessary to break the bones of the spine is quite substantial. However, in people with osteoporosis, the stress required for the fracture can be minimal – as little as standing for extended periods of time.
Are There Ways to Reduce the Risk of Spinal Osteoporosis?
The equation is rather simple: increase bone density to reduce the risk of spinal osteoporosis.
The most common element required is calcium – the core material of bones. As children, we drank milk to get not only the calcium our bones need, but also the vitamins and trace minerals that better activate the healthy actions of the calcium.
After we pass our mid-30’s, our natural body bone-building machinery starts to not only stop working, but actually go into reverse. We lose about 1% bone density per year after age 35. (Postmenopausal women can lose as much as 5% per year.)
It’s easy to see that taking action soon after that 40th birthday is your best course for risk reduction.
Clinically supported is the combination of AlgaeCal Plus and Strontium Boost.
AlgaeCal Plus has the additional benefit of being plant-based, and ingesting a natural plant source of calcium is always better than rock-based calcium. AlgaeCal Plus adds Vitamin D and K2, plus magnesium. These three ingredients facilitate the delivery of the calcium directly to the bone and the increases the absorption and retention of calcium in your body.
Strontium Boost delivers exactly what the label says: a boost of strontium to your bones. This element is critical in building, and rebuilding, bone density.
And here’s a little extra bonus…
These products not only reduce your risk of developing spinal osteoporosis, but can actually help you recover more quickly from bone density loss – even help you recover more quickly from spinal fractures.
We recommend you check out AlgaeCal Plus and Strontium Boost when you click here.
Sources:
- Melton LJ, 3rd, Chrischilles EA, Cooper C, et al. (1992) Perspective. How many women have osteoporosis? J Bone Miner Res 7:1005.
- Kaptoge S, Armbrecht G, Felsenberg D, et al. (2004) When should the doctor order a spine X-ray? Identifying vertebral fractures for osteoporosis care: results from the European Prospective Osteoporosis Study (EPOS). J Bone Miner Res 19:1982.
- Nevitt MC, Ettinger B, Black DM, et al. (1998) The association of radiographically detected vertebral fractures with back pain and function: a prospective study. Ann Intern Med 128:793.
- Lips P, Cooper C, Agnusdei D, et al. (1999) Quality of life in patients with vertebral fractures: validation of the Quality of Life Questionnaire of the European Foundation for Osteoporosis (QUALEFFO). Working Party for Quality of Life of the European Foundation for Osteoporosis. Osteoporos Int 10:150.
- Pluijm SM, Dik MG, Jonker C, et al. (2002) Effects of gender and age on the association of apolipoprotein Eepsilon4 with bone mineral density, bone turnover and the risk of fractures in older people. Osteoporos Int 13:701.
- Gold DT (2001) The nonskeletal consequences of osteoporotic fractures. Psychologic and social outcomes. Rheum Dis Clin North Am 27:255.
- Robbins J, Hirsch C, Whitmer R, et al. (2001) The association of bone mineral density and depression in an older population. J Am Geriatr Soc 49:732.
- Lyles KW (2001) Osteoporosis and depression: shedding more light upon a complex relationship. J Am Geriatr Soc 49:827.
- Tosteson AN, Gabriel SE, Grove MR, et al. (2001) Impact of hip and vertebral fractures on quality-adjusted life years. Osteoporos Int 12:1042.
- Hall SE, Criddle RA, Comito TL, Prince RL (1999) A case-control study of quality of life and functional impairment in women with long-standing vertebral osteoporotic fracture. Osteoporos Int 9:508.
- Adachi JD, Ioannidis G, Olszynski WP, et al. (2002) The impact of incident vertebral and non-vertebral fractures on health related quality of life in postmenopausal women. BMC Musculoskelet Disord 3:11.
- Johnell O, Oden A, Caulin F, Kanis JA (2001) Acute and long-term increase in fracture risk after hospitalization for vertebral fracture. Osteoporos Int 12:207.
- Lindsay R, Silverman SL, Cooper C, et al. (2001) Risk of new vertebral fracture in the year following a fracture. JAMA 285:320.
- Roux C, Fechtenbaum J, Kolta S, et al. (2007) Mild prevalent and incident vertebral fractures are risk factors for new fractures. Osteoporos Int 18:1617.
- Cooper C, Atkinson EJ, O’Fallon WM, Melton LJ, 3rd (1992) Incidence of clinically diagnosed vertebral fractures: a population-based study in Rochester, Minnesota, 1985-1989. J Bone Miner Res 7:221.
- Delmas PD, van de Langerijt L, Watts NB, et al. (2005) Underdiagnosis of vertebral fractures is a worldwide problem: the IMPACT study. J Bone Miner Res 20:557.
- spineuniverse.com/anatomy/glossary-spinal-terms





Pat linton
May 14, 2016 , 6:10 amMy mother died of an osteoporosis related death. I have been diagnosed with osteoporosis of the spine at the age of 58. I believe in treating this through Pilates and supplements,etc and I really want to continue to use your products. But I struggle with the idea of the lanolin in your products.
I would really would look Iove if you offered algae Cal without vitamin d unless it was vit d2 or lichen based d3. Help?